This is a great example of people not understanding cause and effect.

Allow me to set the table.
It is without question that all academic organizations are desperately looking for that elusive successful black student. They go out of their way to admit blacks, often passing over more qualified and prepared White and Asian students, for no reason other than to stack their student demographics with more black and brown students at the cost of fewer Whites and Asians. This as we have been told for decades is inherently an unqualified good. Whether these students are qualified or suited to their field is irrelevant, all that matters is “representation”, a fancy term that simply means “more spots for people who aren’t White”.
This is even true in academic fields that once were largely immune to this crap, primarily because people die if you screwed up in these fields: engineering, chemistry, aeronautics, especially medicine. If your Uber Eats driver is incompetent you get the wrong sammich. If your neurosurgeon is incompetent? You can end up a vegetable or dead.
Despite this (because of this?), the network of medical schools across America that were once tasked with the initial training of the people who would be the healers of our society have instead fallen into the same mindset of the rest of academia, emphasizing “racial justice” and other nonsensical notions.
It is not debatable that less qualified black and brown applicants are admitted to medical school compared to White and Asian students. The medical school application process is quite different from applying to an undergrad degree program. Prospective medical school applicants use an online portal provided by the AAMC (Association of American Medical Colleges) called the American Medical College Application Service (AMCAS). It is a one stop shop, so your verified MCAT scores are loaded into the system, letters of recommendation, transcripts, etc. You pick the schools you want to apply to and simply submit your application through this portal. It is pretty slick and saves a lot of time, but it also provides a glimpse into the world of medical school applicants and admissions. Here is what we see when it comes to matriculants into American medical schools.

I have shared this before but it is noteworthy and needs to be spread far and wide. What this tells us is that in 2021-2022 the 2,124 black matriculants (those admitted to) medical schools had significantly lower…
– Medical College Admissions Test (MCAT) scores
– Overall GPA
– Science GPA (important to keep pre-med students from loading their schedule with easier non-science classes)
…than any other racial group except American Indians and Eskimos, but their sample size is only 40 matriculants total. Here is a similar graph, I didn’t put this together so I haven’t verified the information but it looks correct (the MCAT scoring is different now):
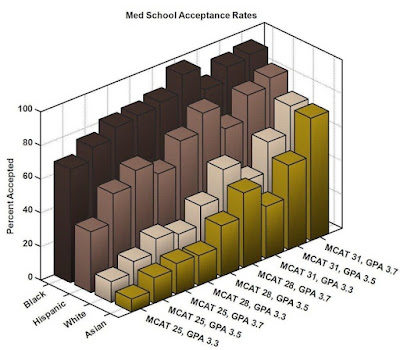
Something else I found interesting. According to the 2020 U.S. census, around 18% of Americans self-identify as “Hispanic or Latino” while only around 12% identify primarily as black. The percentage likely goes up for younger people as the black percentage in America has stayed fairly static for a long time.

Around 9.3% of med school matriculants are black while less than 7% are “Hispanic or Latino” even though mestizo applicants have higher overall GPAs, science GPAs and MCAT scores than blacks. Mestizos also apply at much lower rates, from the above data there were 4,039 mestizo applicants versus 6,169 black applicants. Why are blacks being pushed into medical school while mestizos are not?
Something else interesting to note. According to what is reported by the AMCAS, the schools considered the most elite have higher than average percentages of black matriculants. In 2021, Johns Hopkins first year class had 14 black students out of a total of 120, or 11.6%. Harvard in 2021 reported 16 of 164 matriculants or around 10%. Stanford was 15 of 90 or a whopping 16.6%, up from only 7 matriculants just as recently as 2018 and more than half the percentage of Whites with 27 matriculants. The University of Michigan boasted 23 blacks in 2021 out of 170, or 13.5%. Meanwhile our Indiana system shows 33 blacks out of 366, or just 9% (Indiana’s medical schools are all combined under Indiana University). What were once the best schools have a higher percentage of black matriculants even though blacks on average have lower scores, and I would be willing to be all the money I have that the black students being admitted to Johns Hopkins and Harvard have significantly lower scores and GPAs than White and Asian students who were passed over.
What this demonstrates is that in medicine, perhaps the most critical academic profession, less qualified candidates are being selected for no reason other than their race while other, more qualified candidates, are passed over also for no reason other than their race. We have personal experience with this.
I wasn’t able to readily find statistics for med school graduation rates by race. I suspect that despite overt attempts to push black and brown med school students through the program, that the attrition rate for black and brown medical school students mirrors that of undergrad retention rates by race. I have written about this before, see: Participation Ribbon Egalitarianism Has No Place In Education and also More On Educational Egalitarianism but in a nutshell, even as we have pushed more and more blacks into college, the results continue to be awful with nearly 60% of black undergraduate matriculants having failed to complete their degree after six years.
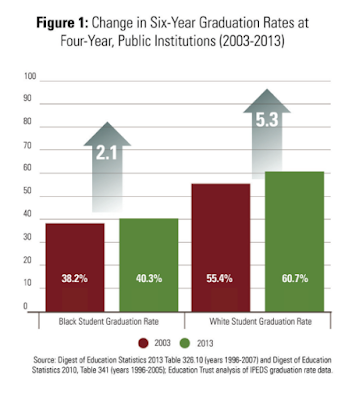
I am sure the medical school washout rate is much lower but I also am confident that the completion rate for blacks in medical school trails Whites and Asians by a not-insignificant margin.

Back to the article. It is written by Usha Lee McFarling (see giant teeth to the left) and focuses on the high rates of dropping out or dismissal of black residents. As this is 2022, of course the only possible explanation is RAYCISMZ!
A STAT investigation found that Black residents either leave or are terminated from training programs at far higher rates than white residents. The result of this culling — long hidden, dismissed, and ignored by the larger medical establishment — is that many Black physicians have been unable to enter lucrative and extremely white specialties such as neurosurgery, dermatology, or plastic surgery. It’s a key reason these fields have been unable to significantly diversify their ranks even as the total number of residency spots has increased nationally.
Medical school is highly competitive and very stressful, and that is intentional. So is residency. That is by design as being a doctor means making decisions, often very quickly, that have life and death consequences. This is especially true as you get into the more challenging, and therefore more lucrative, specialties. The system is designed to weed out people who can’t hack it. It used to be that we appreciated this as a people, no one wants a brain surgeon who freezes up under pressure. My dad told me about his experience in medical school many years ago and it was a lot of messing with their minds to cull the weak. There is less of that now and the medical profession has suffered for it.
The article starts out with the story of Rosandra Daywalker:
Rosandra Daywalker had always excelled. The daughter of Haitian and Jamaican parents in Miami — one an auto parts clerk, the other a nurse — she’d received a nearly perfect score on the SAT, earned a full academic scholarship to the University of Miami, graduated summa cum laude from Morehouse Medical School, and was inducted into the prestigious Alpha Omega Alpha medical honor society.
Then came the icing on the cake: She matched into the elite and highly competitive specialty of otolaryngology, a field she’d fallen for after watching an elegant head-and-neck cadaver dissection in medical school. Standing on the stage during Morehouse’s Match Day festivities in 2015, Daywalker beamed. Her family could not have been more proud. The fact that fewer than 1% of otolaryngologists are Black seemed a distant concern.
A couple of things jumped out at me immediately. She got a “nearly perfect score on the SAT” but what does that mean? It could mean a lot of things but we just simply don’t know. Then were are told she received a “full academic scholarship” to the University of Miami, hardly an elite school by any measure, before going on to medical school at Morehouse Medical School. Morehouse is a historically black college and while I don’t have access to the full profiles of med schools including average GPA and MCAT scores, I did at one point and you will have to take my word for it that the historically black college medical schools weren’t getting the best and brightest.
She finally matched into otolaryngology, basically head and neck, which is a very competitive field. That is when things started to go wrong and we get a clue right away
But when her supportive female program director left, everything changed. Suddenly, Daywalker could do no right. She was told she wasn’t closing clinic notes fast enough, even though she thought she closed them as quickly as other residents. She was told to be on campus all day even though other residents often worked from home. Her previously excellent performance reviews dropped in every area. According to a lawsuit Daywalker brought against UTMB, she was intimidated in the operating room, denied rotations she requested, falsely accused of posing safety issues, subject to faculty members’ hostile comments about Black and Hispanic patients, and retaliated against for raising concerns about how a Black patient was treated.
Her supportive female program director left and now on her own she couldn’t hack it. Notice lines like this:
She was told she wasn’t closing clinic notes fast enough, even though she thought she closed them as quickly as other residents.
She *thought* she was closing them fast enough, meaning that she wasn’t. Pretty quickly she started to unravel, having panic attacks and then going on medical leave. In other words, the rigors of the program caught up to her after her “supportive female program director” wasn’t around to run cover for her. Eventually she left the residency and of course is now suing the University of Texas Medical Branch at Galveston because her failure must be their fault. Also of interest was this blurb from the response to her suit:

Rosandra Daywalker sounds like a perfectly rational and balanced person that I definitely would want performing surgery on unimportant body parts like the head and neck.
The rest of the article are sob stories from blacks who couldn’t hack it in their residency programs. There are lots of them, highlights in red mine:
Data on residency dismissal by race have not been routinely collected by national medical organizations and are frustratingly difficult to locate. But the few numbers STAT could find are startling and lopsided: While Black residents account for about 5% of all residents, they accounted for nearly 20% of those who were dismissed in 2015, according to an unpublished analysis by the Accreditation Council for Graduate Medical Education.
That analysis showed that in every field examined, including specialties that have historically been more welcoming to Black physicians such as family medicine and pediatrics, Black residents were dismissed at rates higher than white residents. The same analysis showed that within the field of surgery, 12% of Black residents were dismissed in 2015, while just 2% of white residents were. (ACGME officials cautioned that the analysis should be viewed with caution because the numbers of Black trainees is so small.)
In the more elite medical specialties, the numbers may be even bleaker. A 2020 paper found that people from groups underrepresented in medicine make up 6% of residents in orthopedic surgery, but 17% of those dismissed. In neurosurgery, the numbers terminated some years are higher than 20%, said Owoicho Adogwa, an assistant professor of clinical neurosurgery at the University of Cincinnati who last year co-founded the American Society of Black Neurosurgeons to help stem high attrition rates. Only a handful of those who leave neurosurgery training programs are able to find spots in new ones, he said. Most switch to other specialties, often non-surgical, while some leave medicine altogether, still carrying the massive debt of their medical school loans.
Clearly there is a pattern to be noticed. All across the spectrum, blacks are washing out of residency at much higher rates than Whites. The question is why this is happening. Ms. Usha Lee McFarling thinks she knows, and I am sure she decided this long before she started writing: RACISM!
That is of course not the only possible explanation or even the most plausible.
We have already seen that blacks with lower qualifications are being admitted to medical school in contrast with their White and Asian peers.
Shockingly, when these black and brown matriculants get through the academic portion of schools and away from the protective cocoon of sympathetic faculty and staff in a university setting, they seem to founder. Steve Sailer put it nicely….
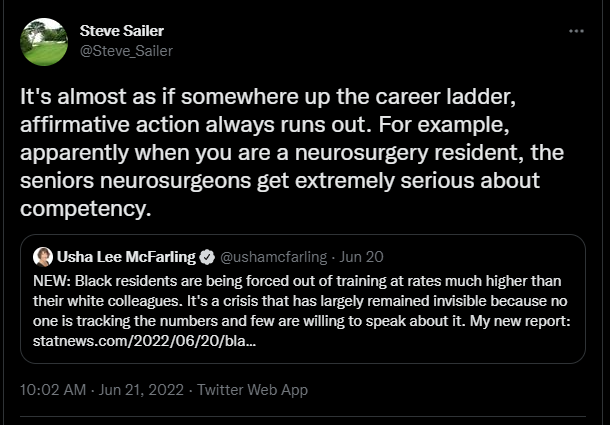
Perhaps you could add in that people who have impulse control issues as a group might not be as well suited to occupations where high, constant stress levels are commonplace. Not everyone is suited to every job. I always thought I would follow in my father’s footsteps and become a doctor but apparently if you can’t stand the sight of blood and are terrible at math, it cuts your medical school dreams short in a hurry. I am not suited to being a doctor or any number of other professions from engineering to the NBA. That isn’t unfair, it is simply how it is so I chose to do things that do suit my particular skill set. That is part of being an adult.
When you flood the pipeline of medical students with matriculants who are not up to par with their peers, it is inevitable that you will see much higher attrition rates along the way, both in medical school and later in their career path. It is unfair to those washing out, not because it is “racist”, but instead because mostly White liberals have set them up to fail and if you wash out of medicine after med school, your chances of paying off those big medical school loans gets much lower.
Not to worry though, the same author of the original report published a follow-up report the next day:
What will it take to level the playing field for Black residents?
You can probably already guess. Her recommendations are….
Collect the data, which means requiring onerous reporting for residency terminations by race:
(Edjah) Nduom’s group is calling for dissemination of national data on residency termination by race and an accounting of residents who are dismissed or withdraw from individual programs so medical students can avoid programs with a poor history of graduating Black residents — and so these programs can be held accountable.
This is rather blatant blackmail. No woke university administration want to see their residency program stand out as one that washes out too many blacks so you can be sure there will be extra pressure to coddle black residents, just as there is throughout the process of becoming a doctor.
Next, improving “protections” for black residents….
(Vanessa) Grubbs’ group plans to stage a demonstration in August to raise awareness about the unjust dismissals of Black doctors and trainees. What’s needed, she said, are firm due process guidelines, and sanctions from ACGME or even the Centers for Medicaid & Medicare Services, which funds residency programs and used the cudgel of withholding funding to desegregate hospitals in the 1960s.
At the very least, she said, residents should be allowed to have a faculty member or faculty member in the room with them during disciplinary proceedings. “It’s so unfair for a resident to be fighting this by themselves,” she said.
Notice the reference to withholding funding. That is the ultimate stick to bring programs that are not sufficiently woke into line, because those funds are what keeps the administrators pulling down those fat salaries. I GOLd (guffawed out loud) at the idea of residents needing “a faculty member or faculty member in the room”, nice editing job btw, in the room to hold their hands. A resident has completed four years of undergrad and four years of medical school so generally they are at least 26 years old but can’t deal with a disciplinary proceeding without a security blanket. When I was 26 I had been married for six years, been in the workforce for four years and had three children. These residents are incapable of responding to a disciplinary proceeding without a babysitter? I wonder if White and Asian students will get bodyguards or just blacks?
Then we need more “support” instead of “weeding out” of residents. The goal again is not to make sure that the best people are proceeding through the program but instead to make sure more blacks complete the programs, whether they should or not. Patients are going to be the ones who will suffer. Finaly they are urged to “not wait” to ask for “help”.
Shenelle Wilson, an Atlanta pelvic reconstructive surgeon who has set up a program to mentor aspiring urologists, said residents should document everything that happens to them, from achievements and praise they receive, to racist behavior they encounter. “I was raised by a lawyer who made me write down everything,” she said, adding that she used the material to contest claims being made against her, such as not covering shifts for other residents. “I had the receipts. They can be vague in their feedback and criticism, but you have to have 1,000 examples to counter what they say.”
Wilson also advised residents to send regular emails to supervisors asking for feedback and asking specifically if there is anything the resident should address. “If they don’t say anything back, that’s tacit agreement they see nothing wrong,” she said. “Then you’re building your case. You have to craft your story.”
And be sure all of that documentation is going to an outside email, Bradford warned, because one of the first things terminated residents lose is access to their institutional email.
The focus seems to be on “building a case” in case you get in trouble instead of focusing on doing your job, writing down every time you actually do your job and badgering supervisors to get documentation that you are in fact doing your job. Maybe if black residents focused more on their position instead of “building a case” to defend themselves from being disciplined, they wouldn’t be disciplined so often? Just a thought.
Ms. McFarling closes her article with this gem:
In recent years, about 8 students have matched into the nation’s roughly 234 neurosurgery residency spots each season. This year, Nduom, who tracked the numbers on Match Day via the many joyous announcements made on Twitter, said a record high 25 Black candidates had matched. In orthopedic surgery, 53 Black students matched this year. These young doctors are about to start their journey toward becoming specialty physicians.
The question is: Will they be allowed to finish?
Allowed to finish? Talk about your loaded language, as if evil White doctors are simply pointing at black residents and declaring that they may not pass. What is worse is that many or most blacks believe that is the case.
This is in line with the first article where Rosandra Daywalker claimed that her career in otolaryngology was “stolen” from her, rather than her simply not being up to the rigors of the program.
Most medical schools and teaching hospitals seem loaded with wokeness so I am confident that they really, really want to have as many black residents as they can but there are certain minimum standards that simply must be met for people in the medical field. I think any rational person would want it that way, you want your doctor to be the most qualified person to care for you.
An already outsized and rapidly growing area of investment in the medical field is not going toward medical breakthroughs or improving patient care and outcomes. It is instead inwardly focused on the medical community that is perceived as “too White”, a rather odd accusation as virtually all of modern medicine is the result of White physicians and researchers.
One unavoidable result of this effort to darken the American medical community is that patients will assume that a black physician is less qualified than a White or Asian physician, knowing that they have been given advantageous treatment from start to finish. That demeans and diminishes the accomplishments of the many black doctors who did made it on their own but even those blacks doctors seem more interested in racial quotas than they are in recognition for their real accomplishments.
The other, more ominous result, is that the quality of medical care in America will continue to slide downward. How can it not when less qualified applicants are constantly admitted to medical schools and residents who are not suited to a role are pushed through anyway out of fear by administrators that they will look bad in front of their peers at cocktail parties?
Competent medical care is going to become a scarce commodity, so I recommend putting “find a competent middle age White or Asian doctor” on your prepping list.

Wow. Thanks for the eye-opening article Sir. It just so happens I'm currently "in the market" for a new Doc (in the Stanford Health system, no less!), this adds an interesting twist to the search.
Back in the mid/late 80's I had a black GP for a few years. He was…adequate. My choices were between him (who had been practicing 20+ years)and a really young guy that was fresh outta school. While I can't say anything negative about him, when I had to switch docs due to a new insurance company, I shed no tears. And he went through Med School in the late 60's, when their standards were still pretty high.
Nowadays, I mostly stick to Eastern medicine except when absolutely necessary. I haven't been to a "real" (western med) doctor in over 5 years but have an issue that *may* need surgery, thus the search. It's ugly out there trying to find a decent doc these days!
The sickcare industry has brought everything upon itself. Pissing away it's trust not only over the last 2+ years, but stuff like this, about billing and doing things that aren't really helpful but hey, they get paid. (knee surgeries on people 6 months from death, chemo on stage "8" cancer, all the BS meds and meds and meds that clearly don't work and are outrageously priced).
My GAF about the sickcare industry top to bottom is zero and I imagine as more and more people are harmed by the effects of the "safe and effective" treatments of the last few years that people are going to ummmm not be pleased. (must not fedpoast).
I honestly can't wait for it all to burn down and them all to ………………..
Doctors, nurses, the whole kit and caboodle deserves everything that's about to happen to it.
It needs to be acknowledged that at the very high end of intellectual endeavor there will be be fewer blacks than whites or Asians. There will also be fewer women. Complaining about it will not change it. Nothing that we have control over will change it. What can and is being done is pretending that limitations on black intelligence do not exist and to force them into positions where the shortcomings are evident. This helps neither them nor those who become their victims as a result of poor performance. The infatuation with exact numeric percentages in every field (except sports) is not something to be desired
Arthur said: "What this demonstrates is that in medicine, perhaps the most critical academic profession, less qualified candidates are being selected for no reason other than their race while other, more qualified candidates, are passed over also for no reason other than their race. We have personal experience with this."
Could you elaborate on this? Specifically the personal experience part.
Thanks
The bit about closing out case notes in a timely manner struck me, knowing well that the relationship between the various shades of blacks and "time" is a very tenuous thing. My wife spent her career in nursing, most of it in management, and in her universe, dealing with blacks and their "time and attendance" lapses was a recurring nightmare. They simply CANNOT do ANYTHING on the White man's clock. They even joke about it among themselves, saying that they run on "nigga time".
Nurse's aides would show up anywhere from 15 minutes to 2 hours late, "forget" to punch in and demand that their supervisor sign their time card for the precise moment their shift started without them. Then they would leave promptly at the end of their scheduled shift, whether the next nigga in line had shown up to take report or not. Generally, the black nurses were just as bad.
But they always had a "good" excuse. Had to get dem babies off to skoo', or dey was traffic that never seemed to afflict the White girls. It was such an ordeal to write up a chronically late black aide or nurse that the White supervisors just stopped doing it. Very similar to police in the ghetto standing down and not troubling themselves to haul petty black criminals in, knowing that they would be free without bond a couple of hours later. Just not worth the aggravation.
One final thought about "nigga time". My employer, one of the Big Three in defense, updated our yearly ethics training in 2022 to include statements to the effect that employees cannot be held to strict starting times anymore. It is considered harassment and discrimination to expect "other [non-White] cultures" to respect traditional [White] notions of timeliness. They actually depicted a White male yelling at a good, noble black woman while pointing at the clock on the wall in the video, which showed a time of 9:03 if I recall. Yeah, sista was 180 seconds late and Massa Chuck be all up in her bidnez about it. Don't he know it take TIME to get yo' fine glamour on?
Class of 1991 from a Philadelphia medical school, American Asian. Started with a class of 160, about 35 Black students. They had their own tutors extra help etc. About, 20 made it through. Not a great rate but our class valedictorian was a black fellow that matched in orthopedics. My fellow Asians always felt we had higher entrance criteria but couldn’t prove it.
This comment has been removed by the author.
Medicine in this country has been on the downhill slide since Rockefeller medicine came to prominence in the 1920's. The decline was compounded further by the introduction of 'managed care' in the 80's. Today, with the total capitulation of ethics, integrity and morality – a.k.a. the scamdemic – along with the imposition of Social Marxism – of which the transformation of baboons and other untermensch into doctors is but a symptom – it's about to receive it's coup de grace which, in my opinion, is long overdue!
It's no secret that crony capitalism hollowed out and corrupted the institution thus making it ripe for the wokies to go marching through it, and they're high-steppin' big time. Shouldn't be hard to guess where this all winds up – which is why I made a serious effort to take control of my family's health 35 years ago. Intense exercise, healthy food, lots of water, herbs, acupuncture, Traditional Chinese Medicine, supplements, meditation and being a rabid autodidact by nature has kept us far away from that whorehouse of egomaniacal quacks. I go to an integrative medicine doc (paid in cash) once a year for blood and diagnostic tests and relegate any contact with the bordello to trauma/emergency medicine and certain types of surgery.
Yes, the shitlibs will get what they want and dumb down healthcare to the point of total disfunction so, like everything else, withdraw from the system. If you stay in it you get what you deserve – which will most likely include a hostile 'doctor' with a decorative bone in his/her nose.
Get/stay healthy and look to alternative medicine as a viable way to emancipate yourself.
I’m sure those trust falls and kumbaya drum circles between blunt rolling sessions are working out well for you.
I’m an American CAUC-Asian. Do I get any intersectional bonus points?
The comment above from the Asian physician about special tutors and prep classes from blacks is real. I am in a small Southern city that is still considered ground zero for racism and the medical school here is the absolute undisputed center of the politically correct woke universe, and those programs described to coddle black students do indeed exist. White and Asian students cannot access them even if they offer to pay extra. It's been that way for over two decades.
And I see the results in my ER. Zero diagnostic skills, zero interest, zero curiosity, as brilliant as a polished turd.
Don't forget to include the high levels of middle eastern and indian (dot, not feather) doctors flooding our shores. UTMB is covered up with them. We recently had to change doctors due to insurance issues, got a list of approved doctors and maybe 1 in 10 had a recognizable American name. The rest? Shwarma Muhammad Goatfucker was way more typical. Finally got insurance settled and and went back to the Asian female doctor we initially had and liked very much.
I'm assuming, don't know out right, but assuming that most did their undergrad work overseas and maybe some medical, only finishing up here in order to practice? From the thick accents of the few I had to see, it was obvious they weren't born here. Fun times. I'd almost trust voodoo medicine over some of the shit my wife had to go thru.
Been practicing medicine for nearly 50 years. Even back in the 70s, the affirmative action students and physicians were mediocre. Over my entire career (roughly half Ivy League academic, half Appalachian private practice), I've encountered maybe 2 or 3 impressive black physicians. With all the woke nonsense and the dumbed-down curricula that students now get K-12-college-med school, the white kids are getting less and less competent by the year. My best advice is to find yourself an old physician.
First off, my wife has two east Asian doctors. Her pulmonologist is from India and still has the thick accent, but she has been seeing him for 20 plus years. He's a good doctor. Her other doctor is from Pakistan and is the one who caught her cancer at stage one, effectively saving her life. I don't know, nor care where they went to med school. Anecdotal to be sure, but that is our experience.
On the other hand, perhaps these "affirmative action" med school students, residents and new doctors can practice in their respective demographic areas and see if their fellow racial demographic will see them for their medical care. That's where the rubber hits the road.
We did even better and grew our own, she is just finished with her second year and started her clinical rotation.
The East Asian docs we have encountered a pretty decent, the accent can be a problem but they seem competent but I wouldn't see a black physician under 60 for any reason
There are a lot of specialties, esp in urban system, where you can barely get an American doc. It seems like most of the White kids either go into family practice/OB-GYN/pediatrics or a handful of specialties like orthopedic surgery.
Med school is really weird now, our daughter just finished M2 and is onto clinicals and it seems to me like they spent very little time actually learning anything for the first two years. Partly because of Covid, but the schedule really strikes me as odd.
Asian
Asian
Asian
Art forgive me, been busy prepping the house for sale so not here as often as I'd like. Even today I'm procrastinating.
I was linked to you from WRSA and wow what a hell of a write up. Been there done that.
My daughter had a brain tumor 2 years ago. She's fine now but in my fog I would talk to a few acquaintances about it before the surgery. My favorite was a lady in Walmart (now retired, to much cover bullshit) she ran the sporting goods desk so I saw her pretty often. She told me about a niece that was messed up in her surgery.
Divine intervention through a neighbor led me away from the top surgeon in Tulsa to Dr. Cohen, pediatric neurosurgeon John's Hopkins. That is the only hospital I will ever recommend for specialty treatments. Fantastic experience. His office people are special, he even has a rap video funny as hell. He's white and older. His pedigree on his office wall is amazing.
Thank you for what you do.
covid not cover. Phk google. Tried to spell check me again.
Good on her! Let's hope she can stay clear of all this PC and woke nonsense.
I read an article similar to this some years back. It was about how blecks were given rides to colleges that they otherwise wouldn't have qualified and failing. They had copious amounts of sunshine blown up their skirts, only to change majors to angry studies or quit altogether. One of the examples they told about was sort of heartbreaking. This black girl was excited to be pre-med, and her first biology class she was well over her head. Everyone in the class had AP science courses all through high school. She had one. A normal one. She started failing nearly straight away. So at least she realized she was going nowhere early.
Back in the day, I used to deploy networks – from structured cable, to rack and stack, to configuration and setup. I managed all sorts. It was, and still is, a great field. It's where, no matter who you are, if you have some intellect and drive you can do well for yourself. I've managed all types. But it is an alpha dog environment, so you need to work hard and have thick skin to succeed.
My observation of why blecks fail at endeavors like these (medical school, Tech) comes down to two things: Work ethic (theirs' sucks) and misplaced Pride (they won't sacrifice for future gains). Work ethic makes you show up on time, or early, work hard until the job, or work for the day is done. Those that understand they don't know everything, and learn from the more experienced dudes do well. Whites, asians, and hispanics all get that in my field. Basically everyone but blacks, for the most part. They know how the field is striped, and they play the game well. I've seen some really dumb things from black workers – Like above – they work on their own timeline, whatever that is. It seems to change daily. And good lord the excuses. They don't seem to think that they need to check with anyone for a day off. They'd do the bare minimum of work that they needed to get by. I still have friends in those companies. I can tell you one area that they excel – Complaining to HR, claiming victim status.
@Anonymous from 12:48 AM:
And I'm sure the psych meds and third-world hospital staff are keeping you just above room temperature too pally!
Based on the (somewhat inadvertent) disclosure from the Harvard office of undergraduate admissions, the odds of that a black individual in a high-status position got there because of skin color is roughly 97%.
Of 31 black freshman in a recent year, exactly one would have been admitted under standard, merit-based criteria.
Pingback:America Has Too Many Qualified Doctors And Pilots! – Dissident Thoughts
Pingback:Moar Med School Malpractice – Dissident Thoughts